
To kick things off at HealthSpaces (Almost) Live, we brought together a group of senior real estate and facilities leaders for a "State of the Industry" discussion featuring Jeff Land, SVP of National Real Estate for CommonSpirit; Brian Weldy, Vice President of Engineering and Facilities for HCA; and Rick Redetzke, SVP of Facilities and Real Estate for SSM Health. Robert Moss, SVP of ERDMAN, moderated this conversation.
Across the board and with rare exception, health systems are facing the same monumental challenges at this moment. In this wide-ranging conversation, panelists hit on some of the most primary concerns: how they're moving forward (or not) with capital projects and operational expenses at a time of limited resources; how they are reassessing their real estate portfolio when large portions of the workforce are working from home; the impact telehealth will (or won't) have on physical spaces; and what the future holds for healthcare delivery.
As cost pressures continue, Redetzke said, "We just need to simplify and reduce the cost of our real estate portfolio in any way possible."
SSM Health has a lot of legacy real estate as the result of some integration that happened; the same can probably be said for the majority of medium-sized and large health systems today. He's looking at combining locations in markets where there are multiple locations and having maybe one access point instead of the several access points that are legacy in their portfolio.
A major focus of his commitment of capital is to also "be really purposeful with facility infrastructure." They now have a dedicated capital plan that's focused on the things people don't see: mechanical spaces, building enclosures, physical security, and energy efficiency projects.
Having recently completed a half-billion-dollar replacement for an academic medical center as well as six other major greenfield hospital projects over the last decade, Redetzke said he doesn't think that will be their core investment going forward. "We’re going to be investing a ton of dollars in new capacity for inpatient settings, and perhaps some replacements."
Land and Weldy said when the pandemic hit, their systems both hit the pause button on projects that were underway to reassess and re-envision their spending. Weldy said that HCA has started to move forward with projects that were underway once again, from breaking ground on new projects to continuing with facility infrastructure reinvestment like replacing roofs or boilers.
"We find that in the capital investment space it's better to have a consistent spend because those things age over time and we need to continue to keep those facilities running," he said. "As far as the major construction projects that are going to be rolling forward, I think we're going to be looking at that somewhat cautiously."
Land wants to see more investment in technology and "lighter, faster, and smaller venues," while at the same time making sure that infrastructure isn't ignored.
"One thing consistent within our mission is the ability to reach those that are underserved," he said, "so I do see us reaching much farther out with remote monitoring and telemedicine, extending our ability to reach more people and more geographies."
At the outset of the pandemic, every single position that could be transitioned to work from home was. Months later, many of those staff are still working from home, a change that many health systems are making permanent to some degree. Many are implementing a hybrid model of work that includes a couple of days at the office each week and the rest of the time at home. Even those organizations that have reopened their doors to employees are seeing many more than expected still choosing to stay home.
"We've found that people are still tending to work from home more," Weldy said. "For example, I'm in a building of about 500 people and on a daily basis we might have 50 to 60 people that have badged in."
Which means a whole lot of administrative space is now sitting mostly empty. To keep paying the leases and operational costs on barely-occupied buildings would be absurd; now facilities leaders have to reassess their real estate needs based on this drastic drop in use.
Weldy said the work-from-home trend was already happening before COVID-19; now those empty spaces are just more obvious. He sees potentially a 20 to 30 percent reduction in space as a result, reducing departmental footprints and consolidating workspaces so that they are shared and occupied on a rotating basis.
Land said CommonSpirit also had a lot of spaces that were historically underutilized even prior to COVID-19. They are now looking at a three-to-one model for workspaces—one workspace for three people to share on a rotating basis. Being based in California, they are still on strict work-from-home orders, so their current occupancy is "in the high single digits" with "maybe eight percent" of their full workforce coming into work every day. They do not expect that number to be more than 30 to 35 percent "in a steady state."
Over the next 18 months, Land estimates a 60 to 65 percent target reduction of administrative space. In some cases, leases were coming to an end or were close enough that they were able to restructure them. In others, they're consolidating and negotiating with landlords. They've also been aggressively selling excess real estate. As they look at remodels, they're designing spaces with much larger conference rooms and common areas for those times when people do all come together.
Redetzke said that SSM Health was already considering a reduction in the administrative footprint in their master planning prior to COVID-19. Administrative staff are currently spread across multiple buildings, all of which have leases coming up in the next three to four years. Now that these employees are set up with the technology to work effectively from home, they're looking to cut down to about 50 percent of the square footage they currently have today.
Prior to the pandemic, only 11 percent of U.S. customers used telehealth in 2019. In 2020, that number has skyrocketed to 46 percent, according to McKinsey. Some providers are seeing 50 to 175 times the number of patients via telehealth than they did prior to COVID-19. With both providers and patients adapting to this new era of telehealth and seeing its many advantages, the shift to telehealth as a significant mode of healthcare delivery will be permanent and will continue to grow.
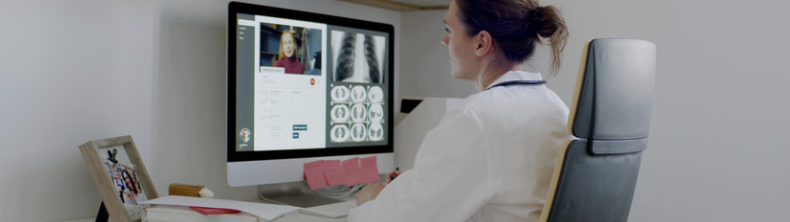
The question for facilities leaders then becomes, how does this massive shift from in-person care to virtual care impact healthcare facilities, and how will facilities need to adapt?
The consensus among the panelists was that telehealth will have some sort of impact on the physical environment, but what that impact will be and to what extent remains to be seen.
"Clearly the consolidation of care models to have physicians who spend part of their day on telehealth and part of their day seeing patients physically changes the footprint for us," Land said. "How exactly I'm not sure yet. I would expect over time to see a consolidation of the number of exam rooms and also changing the configuration of space differently to allow for at least a tenfold increase in our telehealth visits."
And it's not just non-urgent primary care visits and post-op checkups, he said: CommonSpirit is seeing more and more remote monitoring and acute care from home, and has also added a remote behavioral health service to its primary care locations. "This consolidation is a totality of how to manage the patient more effectively."
Likewise, Weldy said that COVID-19 threw HCA into the middle of a drastic acceleration of telehealth adoption, but overall that's a positive change. The next step is to consider how that will impact real estate down the road, but, he said, telehealth is just one component of healthcare.
"You still have to see patients. You still have to deal with things that become acute," he said. "Telehealth will help provide a better way of care in all of our facilities, but it will impact our real estate in some fashion." But for right now, he added, it's just too early to know how much.
It's hard to think 10 years into the future when right now, at this particular moment, planning and predicting even two months out is a challenge. Still, panelists gave their best insights into what this next decade might bring to the future of healthcare, and it's all about accessibility and adaptability.
"We hear two terms a lot: 'resiliency' and 'agility.' Those truly are strategies," Weldy said. "The way we're implementing resiliency right now is we're trying to reduce costs, but the other area is agility, and that is how we are going to move to these news things [like virtual care and healthcare consumerism] quickly so that as an organization we're prepared to do that. How are we helping our organizations be agile during those new discoveries and being someone that can help facilitate that change?"
Redetzke said that buildings have to be flexible and adaptable and, yes, also agile. He believes that the industry is moving more towards outpatient care in different forms, including telehealth, which means a much larger footprint of care at home and maybe smaller points of care for surgeries, specialties, and ancillary services.
But, he cautioned, "You don't want to get too far ahead: land is forever and buildings are for 50-plus years. We can't build something today that's going to be a prediction of what 50 years from now looks like."
For Land, his prediction for CommonSpirit is that 10 years from now is all about "access, access, access."
"It's really about how to reach far greater percentages of the population at far less cost," he said. "When we look at doing that, that means it's going to tread lighter." "Treading lighter" means smaller footprints, shorter leases, and far more technological capabilities to allow for even more advanced remote monitoring and at-home acute care. Land is extremely optimistic about the ways in which technology will allow them to explore different ways to expand remote care.
In short, he summarized, the future of healthcare will be "more retail, more remote, more at-home, more technology, and far more access."

Posted by
A One of a Kind Retreat for Hotel Development, Design & Construction Leaders.
Oct 25-27, 2026 | Fort Lauderdale, FL
Learn more
© Copyright 2025 influence group. All Rights Reserved
Comments